RCM Automation uses powerful AI agents for medical billing to replace manual billing tasks. These AI RCM agents automate eligibility verification, coding, denial follow-ups, and other such tasks to help providers capture up to 20% more of their earned revenue.
|
|
Thank you for Signing Up |

RCM Automation brings together medical billing specialists and AI engineers to build 7 powerful AI agents for RCM. Each AI RCM agent is designed to take over a repetitive billing task, so your staff can spend less time on paperwork.

ELIXA is an AI agent for medical billing that verifies patient eligibility and insurance coverage in real time. By removing manual checks, this AI agent for RCM ensures every claim starts with verified data to reduce rejections.
PRIA acts as an AI agent for RCM that automates prior-authorization requests and payer follow-ups. This medical billing automation tool tracks approvals and helps patients receive care faster without billing bottlenecks.
This intelligent AI billing agent applies CPT and ICD-10 rules with precision. It continuously updates coding logic, improves compliance, and selects the most accurate codes to get providers reimbursed correctly.
With this AI agent for medical billing, you can handle claim creation, scrubbing, and submission. It catches errors before claims go out, delivering payer-ready claims that get paid faster.
DEXA is an advanced AI RCM agent that analyzes denial patterns, generates appeals automatically, and prevents repeat denials. It learns from payer behavior to recover lost revenue and increase future claim success.
Using this AI agent for RCM, you can automate A/R follow-ups to focus on high-value claims. By keeping payers engaged, this RCM automation agent shortens payment cycles and stops revenue from slipping through the cracks.
REMITA is a smart AI agent for medical billing that posts payments, reconciles remittances, and flags discrepancies in real time. This medical billing automation tool gives you a clear picture of your revenue the moment payments arrive.
Let RCM Automation take over your billing and turn delays into dependable revenue.
Here’s why your practice needs them:
Front-End Errors : 60 to 70% of registration-related denials come from eligibility and benefit errors, which AI verification tools can reduce in real time.
Manual Coding Mistakes : Up to 80% of medical bills contain errors, so AI can dramatically reduce these errors through automated coding checks.
Prior Authorizations Delays : Manual authorizations take significant staff hours each week, which RCM automation can reduce by up to 80%, freeing teams to focus on patient care.
Claim Rejections : Integrated AI RCM agents that scrub claims for payer rules can cut rejection rates by up to 18 to 50%, turning more claims into paid revenue faster.

Our AI agents for billing automation are built to move your practice beyond manual billing into a high-performance revenue cycle. These intelligent tools take over complex billing tasks and deliver measurable improvements in accuracy and profitability.
By using advanced claim-scrubbing logic, our AI agents for medical billing catch coding errors, modifier issues, and NCCI conflicts before claims are submitted. This helps practices reach close to 99.99% claim accuracy.
The ELIXA AI billing agent verifies patient eligibility in seconds instead of days. Such agents speed up front-end workflows, prevent avoidable denials, and keep patient care moving without billing delays.
DEXA and ARIS work as powerful AI agents for RCM, identifying stalled or denied claims and resolving them automatically. Practices see over 80% of claims corrected and recovered without staff intervention.
Through complete medical billing automation, our AI agents handle verification, coding, claim validation, and payment posting. This will cut manual work by as much as 70% and reduce dependence on large billing teams.
With continuous automation and optimization, most practices experience 10 to 15% growth in collections within months of deploying our AI RCM agents.
Your dashboard provides live visibility into eligibility rates, payments, appeals, and overall revenue health. Such RCM automation gives your team the insight they need to stay in control of cash flow and performance.
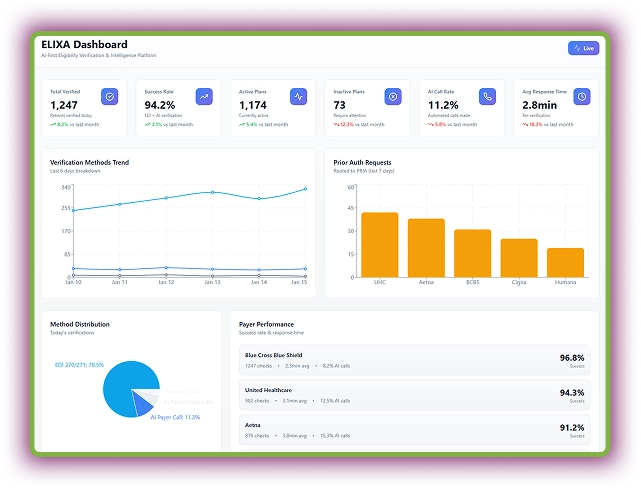
ELIXA transforms eligibility verification with intelligent medical billing automation. It connects to EHRs and payer systems via EDI, APIs, and AI-driven calls to interpret coverage data in real time. It even shows the number of eligibility checks that required prior authorization.
On its dashboard, you can see Live AI Activity to analyze the eligibility verification status happening through billing automation. It even tracks claim details and verification trends.
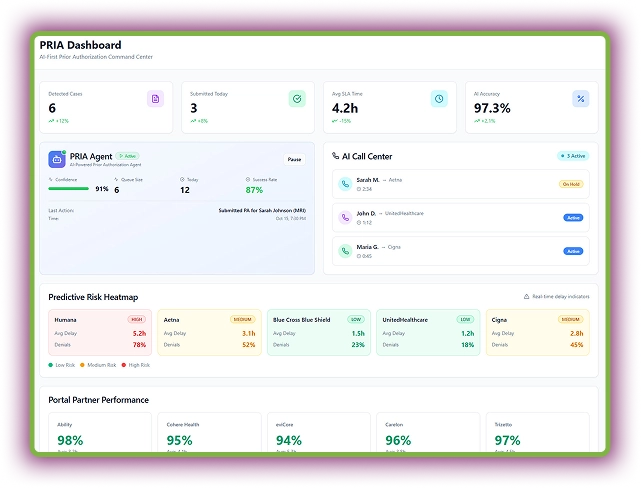
PRIA automates case detection and payer follow-ups with over 97% accuracy. Its Predictive Risk Heatmaps identify high-risk denials before they happen. Moreover, the AI Call Center automates payer calls to drastically reduce manual phone time spent on getting status updates or submitting verbal PAs.
Within the dashboard, you can track integration performance with different payer portals. This agent gives AI confidence in its decision to show it has selected the correct payer.
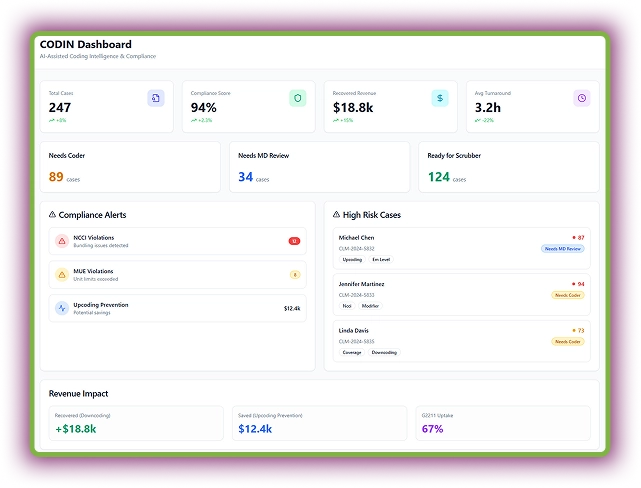
CODIN automates medical coding with AI that reads clinical notes, extracts diagnoses, and procedures. After extracting data points with its OCR technology, matches them to the correct CPT and ICD codes. It audits every claim, detecting NCCI or MUE violations and flagging missing documentation.
Moreover, this medical billing automation agent analyzes prepared claims to suggest the right codes for higher reimbursements.
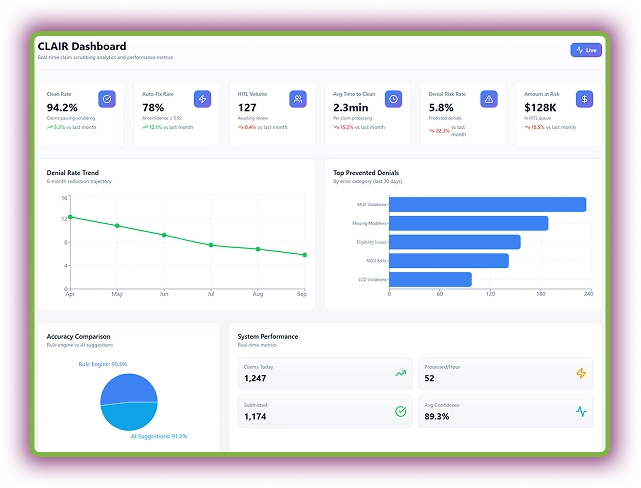
CLAIR is your intelligent claim scrubbing AI agent designed to eliminate denials before they happen. It analyzes claim line items (codes, modifiers, coverage, provider info) using AI and payer rules. The dashboard even displays live clean rates, denial trends, and system accuracy.
Surprisingly, this AI agent auto-fixes minor issues like modifier errors or code mismatches using trained models. Moreover, it compares each claim against historical denial patterns.
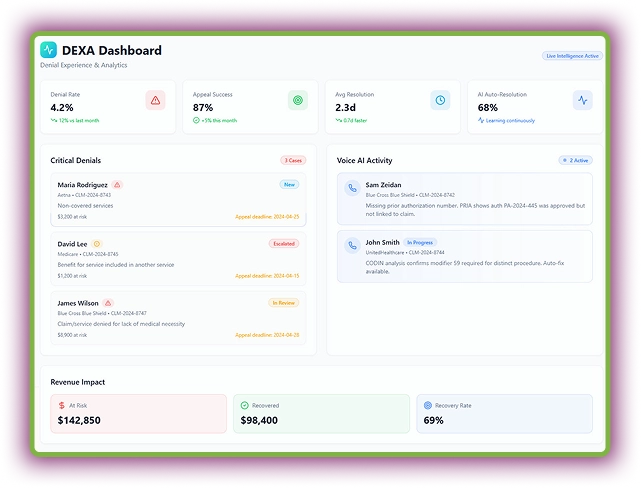
DEXA revolutionizes denial management by turning payer rejections into revenue opportunities. This AI agent detects, analyzes, and resolves denials in real time. DEXA documents each call outcome in real time and updates claim statuses automatically in the EHR or billing software.
More importantly, this AI RCM tool auto-categorizes critical denials, generates appeal letters, and even calls payers to verify claim details.
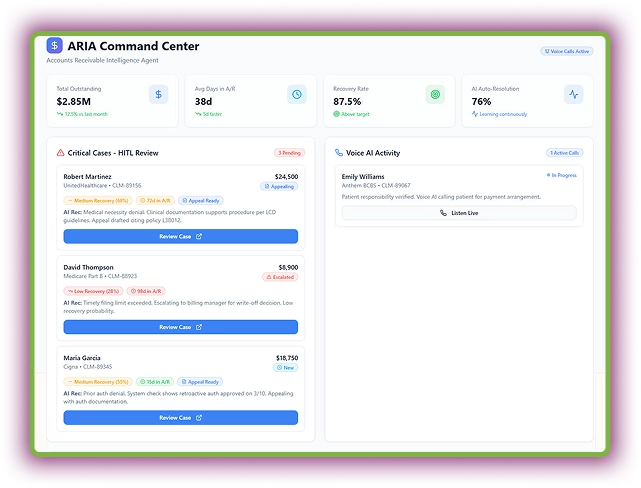
ARIS intelligently tracks outstanding claims and auto-drafts appeals using payer-specific rules. Its predictive engine scores recovery probability, prioritizing the highest-value accounts for faster action. Moreover, Voice AI handles patient payment calls to improve payment collection.
With real-time payer performance insights, ARIS empowers teams to make smarter recovery decisions. Most of the appeals and billing-related escalations are fully automated.
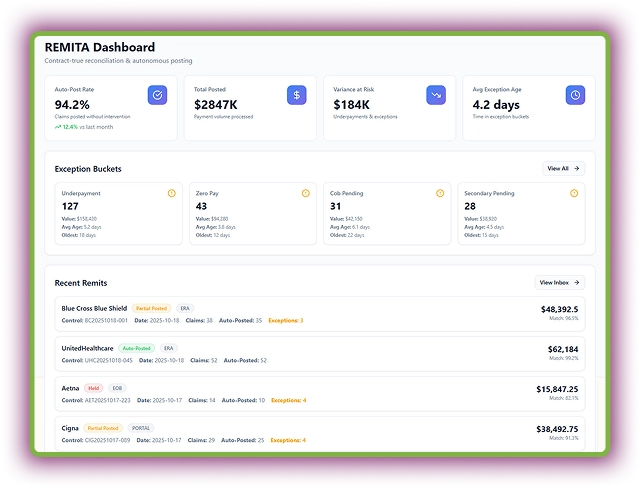
REMITA is an AI automation tool for payment reconciliation and exception management in the healthcare RCM. This AI billing agent auto-reconciles remittance data (ERAs and EOBs) with expected payments and posts payments automatically to patient and insurance accounts.
Plus, this agent detects and flags exceptions, such as underpayments, denials, or missing info. Overall, it reduces manual intervention by continuously learning payer patterns.
AI won’t completely replace medical billers, but it’s transforming their role. Tools like Transcure’s AI RCM agents automate repetitive billing tasks such as eligibility verification, coding, and payment posting. This eliminates manual errors and saves up to 70% of billing time.
However, human expertise remains essential for oversight and strategic decision-making. In short, AI isn’t replacing billers, but it’s empowering them to work smarter.
Yes, Transcure’s AI Agents integrate with most EHRs and payer systems through EDI and API connections for smooth data exchange and real-time updates.
Medical billing automation uses advanced technologies like AI and machine learning to accelerate the entire RCM. Through such a process, you can automate eligibility checks, coding, claim submissions, denials, and payments. It minimizes manual effort, reduces errors, and helps healthcare practices maintain financial accuracy.
All Transcure AI Agents are HIPAA-compliant for end-to-end encryption and full protection of sensitive patient and financial data.
Let RCM Automation take over your billing and turn delays into dependable revenue.